Hormone Replacement Therapy (Menopausal hormone therapy) risks
[A] Combined Oestrogen and Progesterone report
Writing Group for the Women's Health Initiative Investigators. "Risks and Benefits of Estrogen Plus Progestin in Healthy Postmenopausal Women: Principal Results From the Women's Health Initiative Randomized Controlled Trial." JAMA 2002;288:321-333.
[http://jama.ama-assn.org/issues/v288n3/ffull/joc21036.html]
The interim analysis of the Women's Health Initiative (WHI) Trial on the risk-benefit of long-term Hormone Replacement Therapy (HRT) at an average of 5.2 years of follow-up has been reported as:
- Women who took oral oestrogen-progestogen HRT were 26% more likely to have a diagnosis of invasive breast cancer than women who took placebo (relative risk).
- Women who took HRT also had an increased risk of coronary heart disease, stroke and pulmonary embolism
- Women who took HRT had a lower risk of colorectal cancer and hip fracture
- There was no difference in mortality rates between the two groups of women
However, these are relative risks. The absolute risks are minute or statistically insignificant and the study in fact does not show that short-term use for symptom treatment puts women at higher risk of breast cancer or cardiovascular disease.
One can download a PDF version (prints better) at http://jama.ama-assn.org/issues/v288n3/fpdf/joc21036.pdf [I recommend reading the Results, as well as the Abstract which can give the wrong impression taken up by the media, when the facts show that the absolute increases in risks are very small or not significant.]
The Results:
[1] Lipids
The study revealed a 12.7% reduction in LDL-Cholesterol and an increase in HDL-Cholesterol (7.3%) [good so far] but also a 6.9% increase in Triglycerides in the HRT group [unfortunately no data given nor statistical analysis.]
[2] Coronary Heart Disease
A Myocardial Infarction rate of 37 per 10,000 in the HRT group compared to 30 in the placebo group (0.07% absolute increase), reaching "nominal significance" only at the 0.05 level) [A 5% possibility that this could be caused by chance]. The Cumulative Hazard graph [p328] after 6 years shows the difference between the groups rapidly narrowing. [One has to wonder that if the trial had continued, would this small difference have disappeared?]
There was no significant difference in numbers of CHD deaths, CABG or
Angioplasty.
[3] Stroke
29 per 10,000 in the HRT group vs 21 in the placebo group, a 0.08% absolute increase.
[4] Venous Thromboembolism (clots travelling to the
lung)
34 per 10,000 in the HRT group vs 16 in the placebo group, a 0.18% absolute increase. [Not a new finding.]
[5] Breast Cancer
38 per 10,000 in the HRT group vs 30 in the placebo group, a 0.08% absolute increase. This failed to reach statistical significance. [The press continue to trumpet the increased risk, but if we are to believe this study, it is saying that there is no significant risk difference!] The Cumulative Hazard graph [p328] in fact shows a trend to lower breast cancer risk in the first three years.
One possible analysis has suggested the risk was of finding a breast cancer (presumably because of a heightened awareness) but not in breast cancer deaths. In 1998 a large prospective study revealed "that HRT use in women with a family history of breast cancer is not associated with a significantly increased incidence of breast cancer but is associated with a significantly reduced total mortality rate." See Sellers et al Ann Intern Med Dec 1997. Other studies show no increased risk for 5 years and that a "History of HRT use does not affect overall or CHD mortality in women" [Pentti et al Eur J Endocrinol. 2006. In the end, using HRT (especially Oestrogen only in those having had a hysterectomy) for less than 5 years is less worrying than previously thought.
[6] Colorectal Cancer
10 per 10,000 in the HRT group vs 16 in the placebo group, a 0.06% absolute reduction (statistically significant)
[7] Osteoporotic Bone Fracture
147 per 10,000 in the HRT group vs 191 in the placebo group, a 0.44% absolute reduction (statistically significant)
General
These figures are for women averaging 63 years, so for the much lower aged peri-menopausal woman who has very low risk of CHD & stroke, even a relative risk increase of 29% and 41% has little meaning [0 + (40% x 0) = 0]
Global Index (balance of risk/benefit) showed a 0.19% absolute excess risk in the HRT group, but by 6 and 7 years there was no cumulative difference (see graph).[No attempt was made to quantify benefits of HRT for quality of life (symptom control).]
There were no significant differences in mortality or cause of death between groups, but by 6 years there was a Cumulative trend toward more deaths in the placebo group, (see graph) [so if the study had continued, this trend may have made the whole news about HRT risk quite the opposite we have seen!]
Kaplan-Meier Estimates of Cumulative Hazards for Global Index and Death
[JAMA, July 17, 2002 Vol 188(3) pg329]
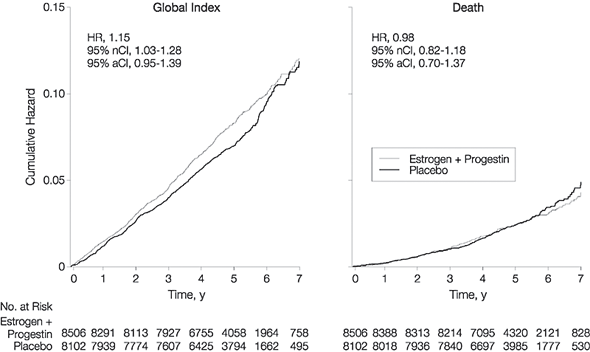
HR indicates hazard ratio; nCI, nominal confidence interval; and aCI, adjusted confidence interval. |
CONCLUSIONS
The conclusions by the authors that the risk-benefit profile of oestrogen-progestin "is not a viable intervention for primary prevention of chronic diseases" is sensible when one is talking Ischaemic Heart Disease, but that doesn't make it as risky as the media frenzy implies [nobody extra died because of HRT, unlike driving in a car!], nor does it appear to prevent women at risk of osteoporosis or colon cancer using it for prevention of those conditions. We still don't know for sure if oestrogen alone (in hysterectomised or Mirena fitted women) can prevent CHD. The study hasn't proven that short term HRT symptom treatment puts women at increased risk of breast cancer or dying of heart disease -however different and lower dose hormones are probably wise! [see the Notelovitz article].
It is unfortunate that the study wasn't designed a bit better or left a bit longer to run. As these women aged, the incidence of dementia, cognitive functioning, independent living, arthritis, depression etc, would have been very important to compare, had the study included some way of monitoring these!
REVIEWS
[B] Oestrogen replacement therapy and Breast Cancer report
Willis DB et al Research Department, American Cancer Society, USA. "Estrogen replacement therapy and risk of fatal breast cancer in a prospective cohort of postmenopausal women in the United States." Cancer Causes Control 1996 Jul;7(4):449-57.
This large prospective US study examined the relationship between fatal breast cancer and use of estrogen (US spelling) replacement therapy (ERT).
After nine years of follow-up, 1,469 breast cancer deaths were observed in a cohort of 422,373 postmenopausal women who were cancer free at study entry and who supplied information on estrogen use. Results, adjusted for 11 other potential risk factors, showed that ever-use of ERT was associated with a significantly decreased risk of fatal breast cancer of 16%. There was a moderate trend of decreasing risk with younger age at first use of ERT. This decreased risk was most pronounced in women who experienced natural menopause before the age of 40 years. There was no discernible trend of increasing risk with duration of use in estrogen users at baseline or former users, nor was there any trend in years since last use in former users. The relationship between ERT and breast cancer mortality differed by age at menarche and by a self-reported history of breast cysts.
No increased risk of fatal breast cancer with ERT was observed with estrogen use status (baseline/former), age at first use, duration of use, or years since last use.
[C] Oestrogen only HRT and Ovarian Cancer
report
This study highlights potential risk following prolonged use of oestrogen-only HRT.
"While the NCI study does not provide a definitive answer, it does suggest that there may be a small increase in the chance of developing ovarian cancer for women who have taken long term oestrogen-only HRT. The study found that in women who had taken oestrogen-only HRT continuously for 10 or more years, ovarian cancer developed in 6 per 10,000 women per year, compared to 4 in 10,000 women per year for women of a similar age who were not taking any form of HRT."
This an absolute increased risk of 0.02%
Ministry of Health spokesperson Dr Jessamine said; "the study contains a number of potential flaws which limit the weight that can be given to the findings. As the study was conducted on patients first treated in the 1970's using higher doses of oestrogen than are used nowadays, it is difficult to extrapolate the findings of this study to patients currently on
oestrogen-only HRT.
Further research is still needed to determine whether the small increase in risk of ovarian cancer reported in this study persists at the lower doses of oestrogen used in modern treatment
regimens."
Oestrogen-only HRT is quite different from the combination HRT that was the subject of the recently published Women's Health Initiative study, as only one hormone (oestrogen) is used. Oestrogen-only HRT is predominately used in NZ only by women who have had a hysterectomy and is used less commonly than combination HRT (oestrogen and progesterone).
[Compiled by Dr K T Blayney]
