- Political preparation:
Budget 2025 is investing $91 million over four years to fund the increased demand for medicines. This is money that could have been spent attracting more doctors into General Practice to reduce the rising ED and Hospital costs but will now be spent on wasted drugs. Not a cent is allowed to compensate General Practice for lost revenue (which will wipe out any increase in capitation PHO practices receive) and it leaves GPs having to deal with more complications from the reduced oversight/care this policy will create. - The Ministry of Health:
The MoH/HNZ Factsheet is of real concern as it continues the mantra of saving money for patients and ignores the potential harm. Most worrying is the first three conditions suggested as suitable for longer prescriptions, namely Asthma, Diabetes and Cardiovascular disease which co-incidentally are the three conditions most often poorly controlled when patients self-manage without GP oversight. - Medical Council Statement: Principles for quality and safe prescribing practice.
See the full "Principles-for-quality-and-safe-prescribing.pdf."
- Appropriate prescribing: Principle 1 - Must assess the person
1. "Prior to prescribing, a prescriber ensures that they have adequately assessed the patient's condition, and/or have adequate knowledge of the patient's condition, and is therefore satisfied that the prescription is in the patient's best interests". - Inappropriate prescribing:
15. "A prescriber recognises that inappropriate prescribing (which may include indiscriminate, excessive, or reckless prescribing) is clinically and ethically unacceptable. It may be harmful to people and society and undermines trust in the health professions and other health practitioners." - Monitoring requirements:
16. "A prescriber ensures that the person understands the treatment plan (including what action to take if they have concerns), how to access and use the prescribed therapeutic products, and any monitoring requirements." and
18. "A prescriber ensures there are appropriate follow up mechanisms in place to monitor the effectiveness and tolerability of treatment, and for the person to raise concerns and/or provide feedback as required." and
19. "....a prescriber [must assess] progress and reviews treatment options with the person, seeking to optimise outcomes. Decisions to continue or modify treatment are based on this review and according to best practice."
Note that the monitoring is by the prescriber, not the dispensing pharmacist. - Safe prescribing:
23. "A prescriber maintains a contemporary knowledge of ... monitoring requirements, ... [and] effectiveness .... of the therapeutic products prescribed."
27. "A prescriber maintains professional independence and ensures that prescribing decisions are based on the best available evidence to ensure safe and effective care."
That evidence is not just published studies but effectiveness in the individual patient and their tolerance to the treatment. It requires an initial "face to face" / "kanohi ki te kanohi" consultation and then reviews which could range from every day, week, or 1 - 3 months. Longer periods are only safe if a patient is stable, on a very safe single medication they have tolerated for a long period under supervision and when there have been no other changes in health (including other medication) or dose. The decision on when a review is needed is decided by the prescriber, not the patient.
"Prescribers will decide what prescription length is best for each person's health needs. They may issue a prescription for up to 12 months, or for a shorter time if that's more suitable." However...
"People will still collect up to three months' worth of medicine at a time from the pharmacy or up to six months of an oral contraceptive." However...
- Controlled drugs remain unchanged. "There are no changes to how long controlled drugs, including Class B opioids, can be prescribed for."
- Special Authority repeats unchanged. Funding only allows dispensing "to complete the balance of up to 3 Months' supply"
- Dispensing funding is restricted to "only a quantity sufficient to provide treatment for a period up to 3 Months in any single dispensing."
- For Community Pharmaceuticals identified in the Schedule without the ❋ or ▲ symbols:
Default dispensing is Monthly Lots, or 10 day Lots for Class B opioid Controlled Drugs. However, 90 day dispensing is allowed for those with limited physical mobility, those living or working over 30 minutes from the nearest pharmacy, if relocating or travelling.
See "Decision on changes to support increased prescription lengths"
- "GPs to use their clinical judgement" as "autonomous clinicians [with the] skill and knowledge to know when longer prescriptions are appropriate for the patient in front of them" and not follow a formulary guide.
- While some patients stand to benefit from 12-month prescribing [from February] "many others could suffer harm."
- "GPs should "adopt their own in-house policy." For many, this might be that more than 3 month prescribing is the exception, not the rule and that more frequent face-to-face reviews will be required to avoid the medical "shopping list" getting too long!
- "Annual consultations are likely to become more complex and time-consuming with 12-month prescriptions...
This adds further pressure to the workload of specialist GPs and increases the risk of important clinical issues being missed." - "You may be eligible for a 12-month prescription" if:
- your condition and dose has been stable for at least 6 months and;
- regular monitoring is unnecessary and;
- the medicine is approved for 12-month prescribing and;
- you agree to a yearly in-person review.
- Controlled medicines or;
- Conditions or medications needing monitoring or;
- If your condition or medication dose has changed within 6 months
Feedback from GPs around the country about prescribing longer than 3 months:
- "This is not appropriate for multiple medications and pathologies, these will generally need 3 monthly review, either in person or a repeat paid prescription"
- "Will be dispensing 3 monthly (or even more frequently)"
- "If a prescription is prescribed for longer than three months, the next script will need to be in a face to face full consultation"
- "Script review face to face must be a full appointment, not tacked onto another problem"
- "Patients are responsible for obtaining timely reviews. Running out will not qualify for [another] 3 month prescription if not appropriate."
[presumably they mean only sufficient medicine will be prescribed until the patient can be seen] - "Patients will need to sign a waiver that they are accepting a longer prescription at their own risk as it is not in keeping with good medical practice."
- "Doing a repeat prescription, while not as safe as a face-to-face consultation, at least makes the GP review the patient's medication regime and takes time and effort, so the prescription fee is not unreasonable."
- "The 12 month prescription will be very rare and only decided by the GP in a face-to-face consultation.".
While I share many similar feelings to my colleagues, there is often a greater motivation in a non-PHO practice to obtain a repeat prescription or next year, a longer prescription without being seen for financial reasons. As our practice is not producing sufficient income to pay the GP, any expectation of lower prescription costs will result in either the practice closing or much higher fees for anyone demanding longer prescriptions, as the reduced cost of the policy is borne entirely by the General Practice and not the government.
Our research has revealed the longer a patient isn't seen, the greater the number of problems that accumulate and the more severe and advanced any illness becomes (if they haven't already needed a trip to the ED).
It is also our experience that many patients who ask for a repeat prescription actually have significant health problems not addressed and when "required" to come for a review are poorly controlled (especially diabetics, asthmatics/bronchitics, and those with Heart Disease or major risk factors for heart disease). As such, it is far better to have more frequent short appointments than to try to squeeze serious issues into a single consultation, even if time was allowed for an extended consult. Therefore our new practice in-house policy may well see more patients restricted to 3 months (or less) before being seen than allowed more than 3 months.
As we are only continuing in practice to improve or maintain the health of our loyal patients, the same principle to our fees applies, namely, if you want cheap medical care, you are free to try a highly funded practice that gives 12-month prescriptions, but it may not be timely or high quality. (See Venn diagram below). Unfortunately, we cannot accept patients back who leave (unless they had moved away from South Taranaki and have returned).
However, if cost is an issue, see the How you can afford quality Medical Care page, where options for low income or high needs patients are described, including a full refund option for those with long-standing (chronic) illness or disability.
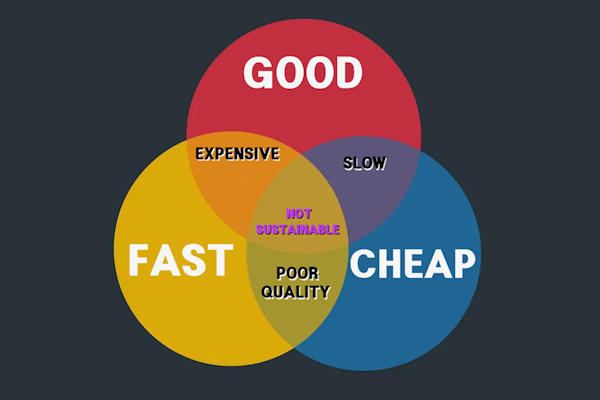 Cheap, Timely or Quality, which two? SPEED - QUALITY - PRICE - Pick any Two. See Wallace's Two-out-of-Three Theory |
 The dilemma |