Vasectomy
Please note that from 2019 I no longer offer Vasectomy services and recommend a Urologist or a GP with "Special Interest" perform this.
General Risk-Benefit
Vasectomy continues to be the safest, most effective and most economical form of surgical contraception producing the fewest complications. More than 500,000 vasectomies are performed in the United States each year. NZ rates have been increasing since 1920 and now 57% of men 40-49 (44% all men >40) have been "done".Large follow-up studies have revealed no overall adverse effects on health following vasectomy, particularly no increase in cardiac risk or cancer death. There were some studies in 1990 suggesting a link with prostate cancer, but prior and subsequent studies have not supported a causative relationship [see literature review]. A large New Zealand study of 923 prostate cancer patients published in the Journal of the American Medical Association (JAMA) of June 19th 2002 concluded that "vasectomy does not increase the risk of prostate cancer, even after 25 years or more". A similar large US Cancer Epidemiology study (1999) found not only no relation, but that vasectomized men who do deveolope prostate cancer present with earlier-stage, lower-grade tumours.
No long-term psychological problems have been found nor any reduced sexual potency or performance.
Failure of the procedure (0.1-1%) may be due to incorrect identification of the vas, (checked by sending a section of vas for histology), recanalization, or the presence of an accessory vas (identified by follow-up sperm counts). In my 38 years of "practising" I have had one failure to clear (accessory vas found on repeat exploration), a few post-op infections, one inability to access the vas, and one persistent pain (later two referred on to a urologist), but no contraceptive failures.
Who?
Patients who seek vasectomy are voluntarily choosing to terminate their fertility and should retain no expectation of fathering children in the future. Vasovasostomy, or "reversal," is expensive and despite a 90% rate of successful surgical reanastomosis, it has a low fertility rate. Basically its a "no return" trip.
Ready?
The patient and his wife or partner should participate in a pre-vasectomy consultation, during which the reasons for the vasectomy are discussed, the method descibed and complications and their avoidance is discussed. An examination of the area is essential.The patient is given a consent form and a list of preoperative instructions. The consent form should be signed (and witnessed) before the surgery. Preoperative instructions should include the scheduling of two to three days of rest following the procedure.
Set
Prior to surgery, a good bath or shower should reduce skin bacterial numbers and a dose of Lorazepam or similar "premed" may be advised to help relax (but this prevents safe driving). I advise either an athletic scotal support or wearing two (new) supporting "jockey" shorts for 24-48 hours after surgery. Shaving isn't usually necessary but you will be advised by the operating doctor.
Surgical Procedure (Go)
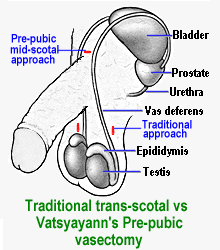
I no longer use a modified Pre-Pubic "Vatsyayann" technique and prefer patients to be seen by a urologist or general surgeon.
The modification I used was to leave the distal (testicular) end untied as this has been shown to reduce postoperative congestive pain and the formation of sperm granuloma (25% with traditional method).
Post-op
Paracetamol or Panadeine and relative rest is recommended with an ice pack and nonsteroidal anti-inflammatory drugs (NSAIDs) if there is any swelling or significant pain. The most common post-vasectomy complication is haematoma (a collection of blood) followed by infection (more likely if there was a haematoma) which is more likely if the patient is too active (so if you get a haematoma, you were probably too active!! - and that includes sex, which is best avoided for a few days and then only tried passively).To ensure the success of the procedure a sperm count is essential after 20 ejaculations (following the laboratory advice on collection) with a second test (to be sure, to be sure). Prior contraceptive methods should continue until the second clear test. Annual tests are recommended for the paranoid as spontaneous recanalization remains a possibility regardless of the technique.